The first coronavirus vaccination in the Republic of Ireland takes place this afternoon
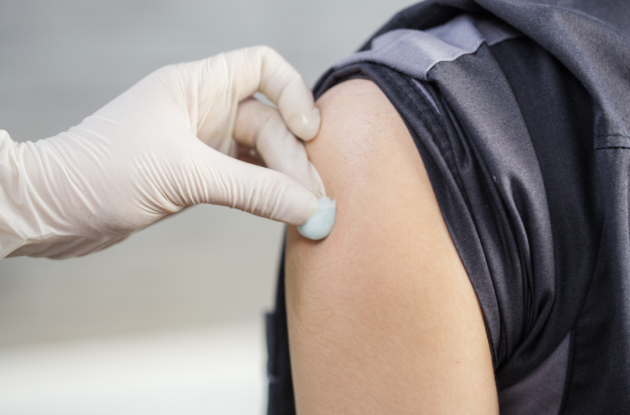
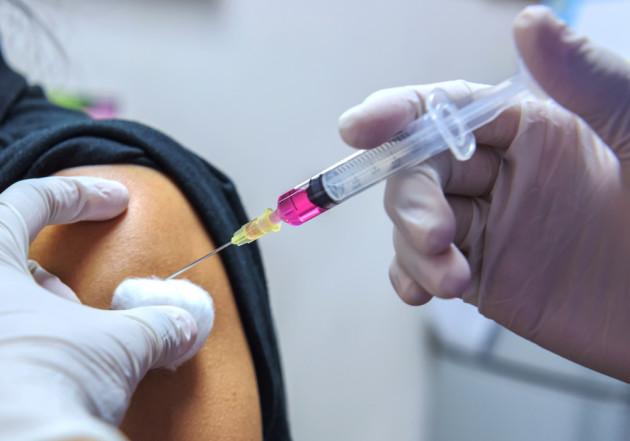
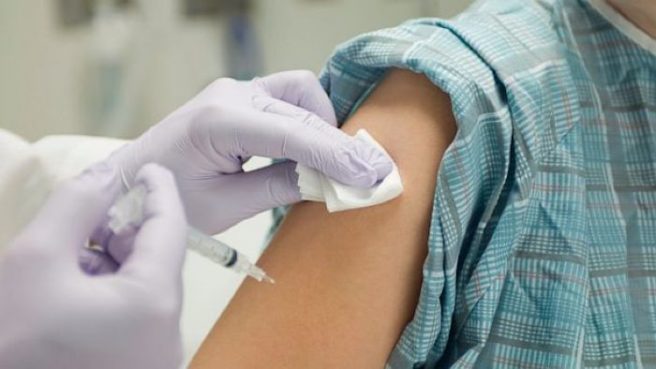
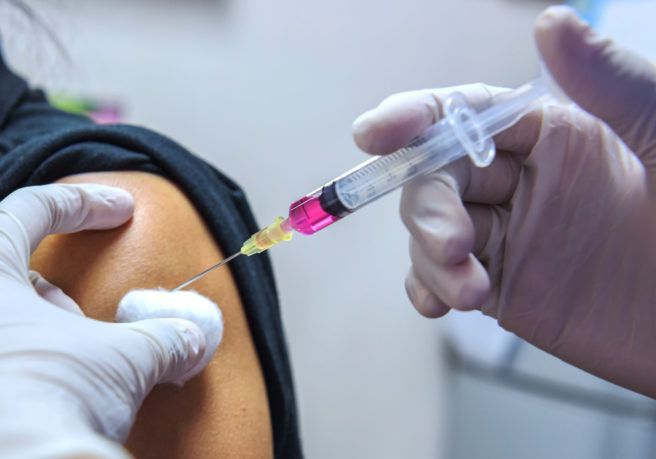
A Dublin woman is set to be the Republic of Ireland’s first recipient of the Covid-19 vaccine, using one of the 10,000 doses of the Pfizer/BioNTech vaccine that arrived in Ireland on St Stephen's Day.
The first few vaccines will distributed in several hospitals around the country, including Dublin's St James' and Beaumont Hospital as well as Cork University and Galway University Hospitals. These vaccines are the first to be given in the nation-wide rollout of the Pfizer vaccine in hospitals this week. This initial rollout precedes the plan to vaccinate in nursing homes next week.
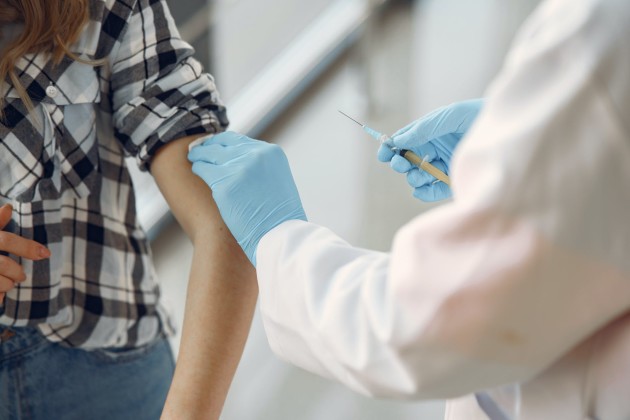
The first person to get the vaccine this afternoon at around 1.30 pm will be Annie, a 79-year-old grandmother from Dublin. Others who will also receive it today includes an ICU nurse, a Covid ward nurse, an allied health professional and a junior doctor.
Head of the vaccine task force, Professor Brian MacCraith. Has said “This is a momentous day. It is the beginning of a complex process, the beginning of the end of an awful period.”.

With 10,000 vaccines currently in the country and 2 doses required per person, this current batch will be able to vaccinate 5,000 people against the virus. 30,000 more doses are due to arrive today.
Brian MacCraith has also said that the AstraZeneca vaccine will be a ‘game changer once it arrives in Ireland, and that he expects by August, anyone who wants a vaccine will have it.
This initial distribution of the vaccine will be given primarily to front-line healthcare workers and elderly people living in nursing homes.
Minister for Health Stephen Donnelly has said this morning: “It’s been the most difficult year for our country. But thanks to the efforts of so many, today we begin to vaccinate the vulnerable and our front-line healthcare workers. Starting with Annie, today we begin a new and hopeful chapter in our fight against Covid-19.”

(Image: Stephen Donnelly Twitter)
The Health Minister posted a photo to his twitter last week and captioned it; "When is a fridge worth photographing? When it's just had Ireland's first Covid vaccines put in it. The first doses have just arrived and many of them are sitting in that very, very cold fridge. We'll begin vaccinating in four days."